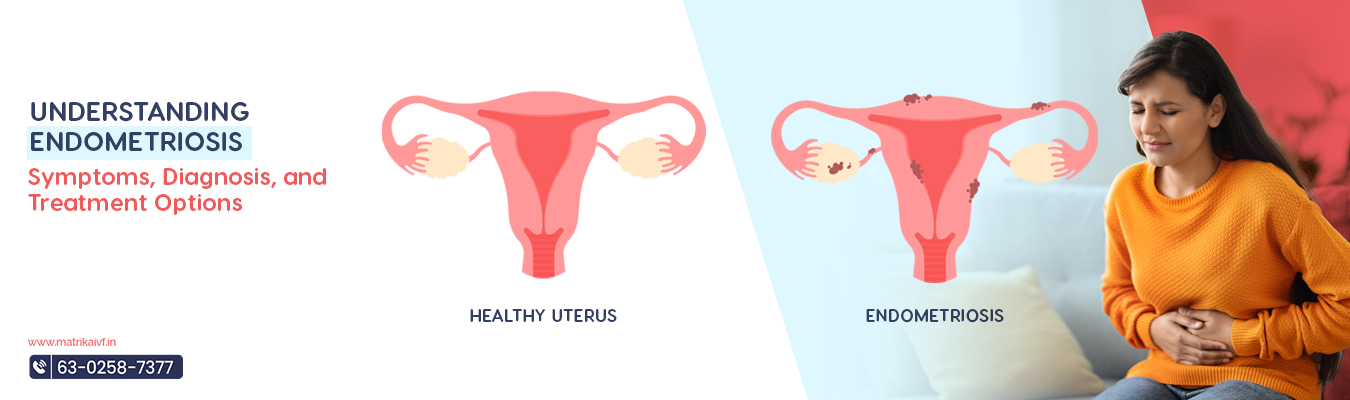
What is Endometriosis?
Endometriosis is a medical condition that affects female reproductive organs. It occurs when tissue similar to the lining of the uterus (endometrium) grows outside the uterus, typically in the pelvic region but can also be found in other areas of the body.
Chronic pelvic pain and infertility are commonly associated with endometriosis, as there is a correlation between endometriosis and fertility issues. Endometrial-like tissue can cover the bowel, ovaries, and tissues lining the pelvis, leading to these symptoms.
While it is rare for the tissue to spread beyond the pelvic area, it is possible in some cases. The endometrial-like tissue that grows outside the uterus is referred to as an endometrial implant.
There are various theories as to why this condition occurs, the cause is not clearly understood.
Endometriosis may cause:
● Inflammation, pain, and lesions
● Irritation
● Scar formation
● Adhesions where tissue binds your pelvic organs together
● Severe pain during the menstrual cycle
● Fertility issues
Notable areas where endometriosis can develop include:
● Outside and back of the uterus
● Fallopian tubes
● Ovaries or Vagina
● Peritoneum (the lining of your abdomen & pelvis)
● Bladder and ureters
● Intestines or Rectum
● Diaphragm (a muscle near the bottom of your chest that helps you properly breathe)
The stages of endometriosis are categorized based on the location, size, number, and depth of endometrial implants. It is divided into four stages:
Stage 1 : Minimal
Stage 2 : Mild
Stage 3 : Moderate
Stage 4 : Severe
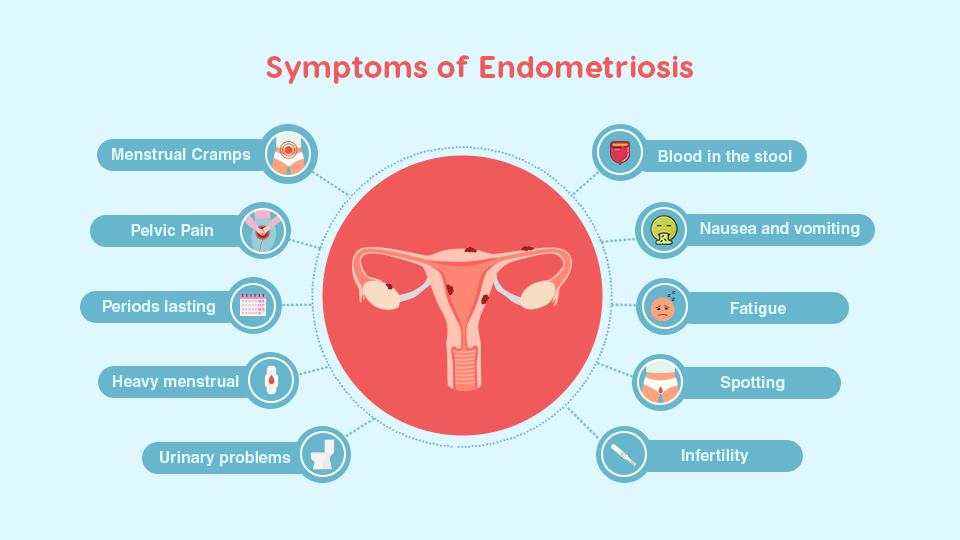
Symptoms of endometriosis may include:
● Painful cramping similar to menstrual cramps
● Long-term lower back and pelvic pain
● Periods lasting more than a week
● Heavy menstrual bleeding
● Bowel and urinary problems such as pain, constipation, diarrhea, and bloating
● Blood in the stool or urine
● Nausea and vomiting
● Pain during sex
● Spotting or bleeding between periods
● Infertility or difficulty getting pregnant
Endometriosis can affect fertility, and pain is the most common indicator of the condition. However, the severity of pain does not always correlate with the extent of the condition.
Pain tends to diminish after menopause when the body stops producing estrogen. Pregnancy may also provide temporary relief from endometriosis symptoms.
Risk Factors & Diagnosis:
Risk factors for endometriosis include age (it primarily affects women in their 30s-40s), a family history of the condition, and a lack of previous pregnancies. Menstrual history, such as shorter cycles, heavier or longer periods, and early onset of menstruation, may also increase the risk.
Diagnosis of endometriosis can be challenging as it shares symptoms with other conditions.
It often takes several years from the onset of symptoms to receive a diagnosis. Diagnostic methods may include a detailed history assessment, physical examination, ultrasound, and laparoscopy.
While there is no cure for endometriosis, various treatment options can help manage the symptoms. Pain relief medications, hormonal treatments, surgery, and fertility treatments like in-vitro fertilization are among the possible options.
Some individuals may also try complementary or alternative treatments and lifestyle changes to alleviate symptoms, although these methods cannot reverse the damage caused by endometriosis.
If you experience any changes in your body, it is recommended to promptly consult a healthcare professional for a proper diagnosis. Working with your healthcare team, you can develop a plan tailored to your specific situation to manage endometriosis and improve your overall well-being.

